Why Do Hemorrhoids Bleed? Hemorrhoids are a very common health issue.
Many people notice blood on toilet paper, bright red blood in stool, or bleeding after wiping, and immediately feel worried.
In many cases, this rectal bleeding comes from bleeding hemorrhoids, also known as piles.
Hemorrhoids are swollen veins in the rectum or anus. When these veins become irritated or damaged, they may start piles bleeding.
This bleeding is usually bright red blood and often appears during or after a bowel movement.
Doctors explain that straining, constipation, pregnancy, prolonged sitting, heavy lifting, and chronic diarrhea are common causes of anal bleeding from hemorrhoids.
Table of Contents
Quick Table
| Topic | Key Information |
|---|---|
| Medical name | Hemorrhoids (Piles) |
| Main symptom | Bright red blood in stool |
| Common sign | Blood on toilet paper |
| Causes | Constipation, straining, pregnancy |
| Types | Internal hemorrhoids, external hemorrhoids |
| Risk factors | Prolonged sitting, heavy lifting |
| Other symptoms | Anal itching, swelling, irritation |
| Treatment | Fiber, creams, sitz bath |
| When to worry | Heavy rectal bleeding or severe pain |
What Are Hemorrhoids?
Hemorrhoids, commonly called piles, are swollen veins in the rectum or anus.
They develop when pressure increases in the lower rectum, causing the veins to stretch, swell, and sometimes rupture.
When this happens, people may notice bleeding hemorrhoids or rectal bleeding.
Hemorrhoids are extremely common. Many adults experience internal hemorrhoids or external hemorrhoids at some point in their lives.
While they can cause discomfort, itching, swelling, and anal bleeding, they are usually not dangerous.
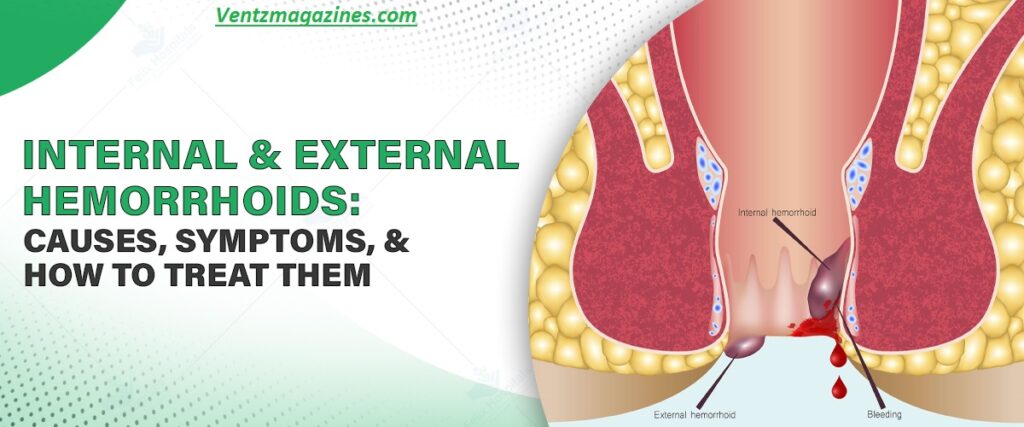
There are two main types:
Internal Hemorrhoids
These develop inside the rectum. They are usually painless but can cause bright red blood in stool or blood on toilet paper. Many people notice bleeding during bowel movements without pain.
External Hemorrhoids
These form under the skin around the anus. They can cause swelling, irritation around the anus, and pain during bowel movement. If the vein ruptures, piles bleeding may occur.
Hemorrhoids often develop due to constipation, straining during bowel movement, pregnancy, prolonged sitting, heavy lifting, or chronic diarrhea. These factors increase pressure on the veins in the rectal area.
When the swollen veins become irritated or injured, bleeding hemorrhoids may occur, which explains why many people see blood on toilet paper or bright red blood stool.

7 Causes of Bleeding Hemorrhoids
Several factors can trigger anal bleeding from hemorrhoids. Doctors commonly identify the following causes.
Straining During Bowel Movements
One of the most common causes of bleeding hemorrhoids is straining during bowel movements. When people push too hard while passing stool, pressure increases in the swollen veins in the rectum.
This pressure can irritate internal hemorrhoids, causing them to tear slightly and bleed. As a result, people may notice bright red blood on toilet paper or blood in stool after using the bathroom.
Straining often occurs when stools are hard or difficult to pass. It can also happen if someone spends too much time sitting on the toilet.
To reduce rectal bleeding, doctors recommend eating more fiber, drinking enough water, and avoiding excessive pushing during bowel movements.
Constipation
Constipation is another major reason why hemorrhoids bleed. When stool becomes hard and dry, it is harder to pass through the rectum. This leads to straining during bowel movement, which irritates the hemorrhoidal veins.
Hard stool can also scrape against internal hemorrhoids, causing small tears and piles bleeding. This often results in blood on toilet paper or bright red blood stool.
People who frequently experience constipation may develop chronic rectal irritation, swelling, and anal itching.
Increasing fiber intake through fruits, vegetables, and whole grains can help soften stool and reduce the risk of bleeding hemorrhoids.
Pregnancy
Pregnancy significantly increases the risk of hemorrhoids and rectal bleeding. During pregnancy, the growing uterus puts pressure on the veins in the rectum and pelvic area.
Hormonal changes also slow digestion, leading to constipation and straining during bowel movements. Both of these factors contribute to piles bleeding.
Pregnant women may also experience anal itching, swelling, irritation around the anus, and discomfort while sitting due to enlarged hemorrhoids.
Fortunately, hemorrhoids caused by pregnancy often improve after childbirth. Eating fiber-rich foods and staying hydrated can reduce the chances of bleeding hemorrhoids during pregnancy.
Thrombosed Hemorrhoid
A thrombosed hemorrhoid occurs when a blood clot forms inside an external hemorrhoid. This condition can cause severe swelling, pain, and anal bleeding.
The clot increases pressure inside the swollen vein, which may cause the hemorrhoid to rupture. When this happens, people may notice sudden bright red blood in stool or blood on toilet paper.
Thrombosed hemorrhoids are often painful and may cause discomfort while sitting or irritation around the anus.
Doctors may recommend treatments such as topical medications, warm sitz baths, or in severe cases minor procedures to relieve the clot and stop the bleeding.
Sitting Too Long
Prolonged sitting, especially on the toilet, can increase pressure in the rectal veins. This pressure weakens the veins and may cause internal hemorrhoids to bleed.
People with desk jobs or sedentary lifestyles are more likely to experience swelling, anal itching, and bleeding hemorrhoids.
Sitting too long also reduces blood circulation in the pelvic area, which can worsen rectal irritation and piles bleeding.
Standing, walking, and taking regular breaks can help reduce pressure on the swollen veins in the rectum and lower the risk of hemorrhoid bleeding.
Heavy Lifting
Lifting heavy objects puts pressure on the abdominal and rectal muscles. This pressure can cause the veins in the rectum to swell, leading to external hemorrhoids or internal hemorrhoids.
When these veins become irritated, anal bleeding or bright red blood stool may occur.
People who regularly lift heavy weights at the gym or perform manual labor are more likely to experience bleeding hemorrhoids.
Using proper lifting techniques and avoiding excessive strain can help prevent damage to the rectal veins.
Chronic Diarrhea
While constipation is a common cause of hemorrhoids, chronic diarrhea can also trigger piles bleeding.
Frequent bowel movements irritate the anal tissues and swollen veins in the rectum, which may lead to inflammation and bleeding.
Constant wiping can also cause irritation around the anus, increasing the risk of anal bleeding and blood on toilet paper.
Managing digestive issues, staying hydrated, and maintaining gut health can help reduce the risk of hemorrhoid bleeding caused by chronic diarrhea.
Symptoms of Bleeding Hemorrhoids
Bleeding hemorrhoids often cause several noticeable symptoms. The most common sign is bright red blood during or after a bowel movement.
People may notice:
- Blood on toilet paper after wiping
- Bright red blood in stool
- Rectal bleeding during bowel movements
- Blood drops in the toilet bowl
- Anal itching
- Swelling around the anus
- Pain during bowel movement
- Irritation around the anus
- Discomfort while sitting
In many cases, internal hemorrhoids bleed without pain because the rectum has fewer pain-sensitive nerves. However, external hemorrhoids may cause pain, swelling, and tenderness.
Some people also feel a lump near the anus, which may indicate an external hemorrhoid or thrombosed hemorrhoid.
While mild piles bleeding is usually harmless, frequent or heavy rectal bleeding should not be ignored.
Is Hemorrhoid Bleeding Dangerous?
In most cases, bleeding hemorrhoids are not dangerous. Small amounts of bright red blood on toilet paper or blood in stool usually occur when hemorrhoids become irritated.
However, persistent or heavy rectal bleeding should always be taken seriously.
Some conditions that may cause similar symptoms include:
- Anal fissures
- Colon polyps
- Inflammatory bowel disease
- Colorectal cancer
Hemorrhoid bleeding typically appears as bright red blood and occurs during bowel movements. Dark or black stool may indicate bleeding higher in the digestive tract.
If hemorrhoids bleed frequently, it may lead to anemia, fatigue, and weakness due to blood loss.
For this reason, medical experts recommend seeing a doctor if anal bleeding continues for several days or becomes severe.
When to See a Doctor
While mild piles bleeding is common, some symptoms require medical attention.
You should see a doctor if you experience:
- Heavy rectal bleeding
- Blood clots in stool
- Severe pain during bowel movement
- Persistent anal swelling
- Dizziness or weakness
- Dark or black stool
- Bleeding that lasts more than one week
Doctors may perform a physical exam or recommend tests such as a colonoscopy to rule out other causes of rectal bleeding.
Early medical evaluation helps ensure that the bleeding is caused by hemorrhoids rather than a more serious condition.
How to Stop Hemorrhoid Bleeding Fast
Stopping bleeding hemorrhoids often involves reducing pressure on the rectal veins and calming inflammation.
Here are effective ways to stop bleeding:
Increase Fiber Intake
Fiber softens stool and prevents straining during bowel movement, which reduces irritation of hemorrhoids.
Drink More Water
Staying hydrated keeps stools soft and helps prevent constipation and piles bleeding.
Use Hemorrhoid Creams
Over-the-counter creams reduce anal itching, swelling, and irritation around the anus.
Sitz Bath
Sitting in warm water for 10–15 minutes helps relax the rectal muscles and reduce rectal swelling.
Avoid Straining
Do not push too hard during bowel movements, as this increases pressure on the swollen veins in the rectum.
These methods can quickly reduce anal bleeding and hemorrhoid discomfort.
Best Home Remedies
Many natural remedies can help relieve bleeding hemorrhoids and anal irritation.
Warm Sitz Bath
Warm water soothes swelling, irritation around the anus, and discomfort while sitting.
Witch Hazel
This natural remedy reduces anal itching and swelling.
Aloe Vera
Aloe vera gel may calm inflammation and help heal irritated tissues.
High-Fiber Diet
Foods like oats, fruits, vegetables, and beans help prevent constipation and straining during bowel movements.
Cold Compress
Applying a cold pack reduces swelling and pain from external hemorrhoids.
These home treatments are effective for mild piles bleeding and rectal irritation.
Prevention Tips
Preventing hemorrhoids is often easier than treating them. Healthy habits can greatly reduce the risk of bleeding hemorrhoids.
Eat More Fiber
Fiber-rich foods prevent constipation and hard stool.
Drink Plenty of Water
Hydration helps maintain healthy digestion.
Avoid Sitting Too Long
Regular movement reduces pressure on the veins in the rectum.
Exercise Regularly
Physical activity improves digestion and reduces rectal pressure.
Do Not Delay Bathroom Visits
Holding stool can cause constipation and straining during bowel movements.
Maintain Healthy Weight
Excess weight increases pressure on the pelvic veins.
Following these tips can prevent anal bleeding, swelling, and hemorrhoid irritation.
FAQs
Why do hemorrhoids bleed when wiping?
Wiping can irritate the swollen veins in the rectum, causing small tears and blood on toilet paper.
Why do hemorrhoids bleed during bowel movements?
Passing stool may damage irritated hemorrhoids, leading to bright red blood in stool.
Are bleeding hemorrhoids painful?
Internal hemorrhoids often bleed without pain, while external hemorrhoids may cause discomfort.
Can hemorrhoids bleed without pain?
Yes. Many people experience rectal bleeding without pain due to internal hemorrhoids.
How long does hemorrhoid bleeding last?
Most minor bleeding stops within a few days with proper care and treatment.
Conclusion
Hemorrhoids are swollen veins in the rectum or anus that can cause bleeding, irritation, and discomfort. Many people notice bright red blood on toilet paper or blood in stool, which can be alarming.
However, in most cases, bleeding hemorrhoids are not dangerous.
The most common causes include constipation, straining during bowel movements, pregnancy, thrombosed hemorrhoids, prolonged sitting, heavy lifting, and chronic diarrhea.
These factors increase pressure on the rectal veins, leading to irritation and piles bleeding.
Typical symptoms include anal itching, swelling, irritation around the anus, pain during bowel movement, and discomfort while sitting.
While mild bleeding is common, persistent or heavy rectal bleeding should always be checked by a doctor.
Fortunately, many cases improve with simple treatments such as increasing fiber intake, drinking more water, taking sitz baths, and using hemorrhoid creams.
Lifestyle changes like regular exercise and avoiding prolonged sitting can also prevent hemorrhoids from returning.
Understanding the causes and symptoms of hemorrhoids helps people manage the condition effectively and reduce the risk of anal bleeding in the future.

